Tendons are a fibrous connective tissue (a bit like a rope) that connect all our muscles to bones, allowing our limbs to move. As our muscles contract and relax, tendons allow the bones to move like a lever. Tendons also play a large role in shock absorption, which helps prevent muscle injuries.
While tendons are super strong and highly resistant to tears, what they don’t do is stretch. Since they’re made up of mostly collagen, tendons are more susceptible to injury if strained or stretched to the point that micro/partial tearing occurs in the rope-like fibers.
Why do tendon injuries occur?
Since tendons are located throughout our bodies, there’s a range of injuries that can occur to these structures. Tendon injuries are also more common as we age and our collagen levels decrease—over time, we’re more likely to sustain micro damage to the fibers in our tendons, which weakens them. The aging process also brings a reduction in blood flow, which is essential for the healing process.
Tendon injuries range from strains, to tendonitis, tendinosis and more (the terms are often interchangeable, and aren’t always doom and gloom). They tend to result from repetitive movements, overuse, and overload, which can cause inflammation and/or weakening of the fibers.
Managing tendon conditions
The first port of call with tendon conditions is to manage the load(s) under which it presents pain and inflammation. Once we’ve identified the cause/load, we make modifications to allow the tendon to settle and become “happier” again. The aim is to keep your pain levels low and stable – below 5/10.
The initial treatment to settle inflammation and reduce pain usually involves manual therapies to help release tight or overloaded muscles. Heat and ice are also great tools for managing inflammation. Keeping the tendons warm by wearing more layers will help them feel more comfortable—this is why pain is often worse first thing in the morning with the first couple steps, or after periods of rest.
We will also likely prescribe an isometric exercise, which is a type of static contraction/hold proven to be effective in reducing inflammation and pain in the tendon—as well as a great start to the next phase of strength building.
Once the pain settles, we move to strengthen the tendon. Tendons don’t get overloaded or overworked without a deficit somewhere along the chain, so we need to identify these deficits to prevent the tendon from becoming overloaded in the first place.
A full functional biomechanical assessment is helpful in identifying any deficits and highlighting where our focus of strengthening should be.
When it comes to progressing tendon rehab and strength, we start with isometrics, then move through range with slow tempos, before increasing weights. We gradually progress the complexity of the exercise—e.g. double leg to single leg—and slowly increase the tempo (incorporating plyometric work) especially if the goal is to return to running or sports.
The table below summarised by ‘Running Physio’ guru Tom Goom (2016) outlines the stages of rehab and progressions when dealing with tendon presentations.
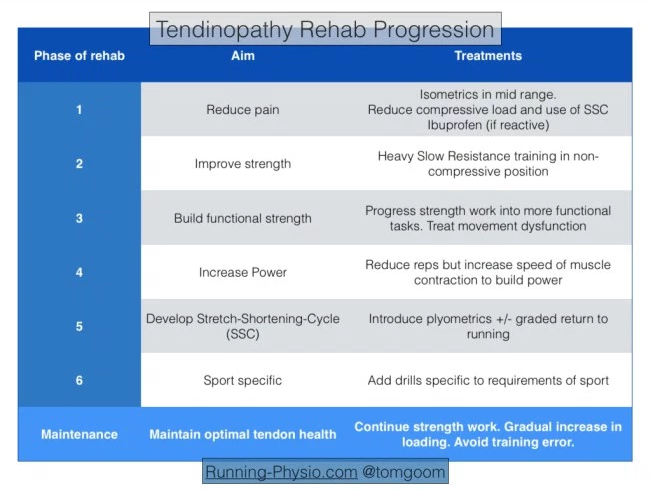
The overarching goal, however, is to improve the capacity of the tendons to sustain higher loads without becoming inflamed and painful. Tendon rehab is essentially progressive overload by adjusting loads, difficulty and speed, but we only ever want to change one variable at a time to avoid overwhelming the tendon and exacerbating the injury. With any progression in your rehab, pain should remain low and stable in the following 24-48 hours. Following a guided and progressive rehab/treatment plan keeps things simple and on track, and more likely to be successful. There is no ‘one size fits all’, so management depends on the level of irritability, current loads, deficits and, of course, the end goal. Therefore, it’s imperative that a full assessment is carried out, so we can look at your daily loads, observe any biomechanical deficits and set you up with a graded rehab program to get you back to doing what you love without pain or recurrence. Get in touch with us today to book in your assessment and let’s get you on the path to being pain-free again.
~ Sophie Alderslade, Physiotherapist
References:
Goom T (2016), Tendinopathy – functional rehab. ‘Tendinopathy – rehab progression – part 1‘.